
1st Trimester Combined Screening for pregnant women – Importance & Benefits
The 1st-trimester combined screening test can detect pregnancies with an elevated risk of trisomy 21 (Down Syndrome) and others like trisomy 18 (Edward Syndrome). The test requires a pregnant woman to undergo an ultrasound between 11 and 13 weeks of gestation & a blood test.
During the ultrasound, the Radiologist takes a measurement of the amount of fluid present at the back of the fetus’s neck, which is called Nuchal Translucency. Although all fetuses at this stage have fluid at the back of their neck, those with Down syndrome, or other Edward syndrome tend to have more fluid.
Furthermore, the Radiologist may also observe the formation or absence of the Nasal Bone during the ultrasound. If the Nasal Bone is missing, there may be an increased likelihood of Down syndrome.
The blood test measures the levels of two distinct chemicals, namely PAPP-A which is a protein & free β-HCG which is a hormone that naturally occurs in the mother’s blood during pregnancy.
Table of Contents
Best time for combined screening
Crown Rump Length (CRL) – min 45mm, max 84mm.
Gestation Age – 11 weeks to 13 weeks 5 days.
Note: After/ from 14 weeks of GA, the NT starts to regress & therefore the biochemical markers (PAPP-A & free β-HCG) will be timed out. These are found to be most sensitive between 10 to 13 weeks.
Importance of 1st trimester combined screening
The 1st trimester combined screening is an important test for all pregnant women to help identify the risk of certain chromosomal abnormalities and other fetal conditions early in pregnancy. This screening test usually occurs between 11 weeks and 13 weeks 5 days, of pregnancy and involves two components:
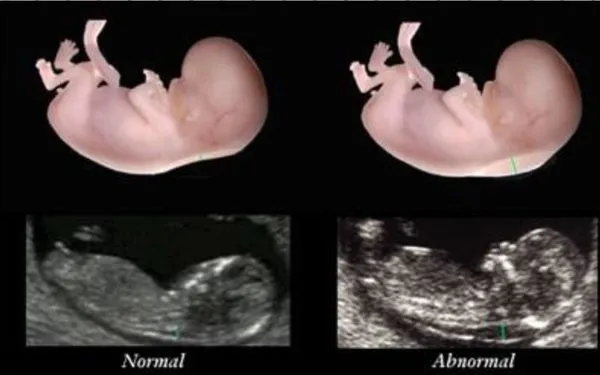
1. Ultrasound: A specialized ultrasound is performed to measure the thickness of the nuchal fold at the back of the fetus’s neck, known as the nuchal translucency. An increased thickness of the nuchal translucency can be a sign of chromosomal abnormalities or other fetal conditions.
2. Double Marker: A blood sample is taken from the mother to measure the levels of Pregnancy-Associated Plasma Protein- type A (PAPP-A) & free β Human Chorionic Gonadotropin (HCG). Abnormal levels of these hormones can also be a sign of chromosomal abnormalities or other fetal conditions.
The 1st trimester combined screening can help identify the risk of certain conditions, including Down syndrome, and other genetic disorders such as – Edwards syndrome & Patau syndrome. If the results of this screening test indicate a higher risk of these conditions, further diagnostic testing may be recommended, such as Chorionic Villus Sampling or Amniocentesis.
It’s important to note that the 1st trimester combined screening cannot diagnose these conditions. Still, it can help identify the risk of these conditions early in pregnancy, allowing for appropriate pregnancy management and counselling.
How 1st trimester combined screening test will be benefited
Screening during the 1st trimester allows doctors & parents to have more time to prepare for or address any potential health issues that their baby may have. However, it’s important to remember that screening tests can have limitations.
For instance, False-positive results may occur when a woman is identified as being at a high risk of having a baby with a chromosomal abnormality, but the baby is ultimately born healthy.
Alternatively, False-negative results may occur when a woman is identified as being at low risk, but the baby is later found to have a chromosomal abnormality.
What you can expect during a screening test
The 1st trimester combined screening involves an Ultrasound Exam and Double Marker Blood Test.
- During the ultrasound exam, an ultrasound probe is moved across her lower belly to create an image of the fetus. The thickness of the amniotic fluid at the back of the baby’s neck is measured, and any extra fluid in this area may suggest a higher risk of a chromosomal disorder.
- Blood samples can be obtained using a syringe for Double Marker tests, to check the levels of protein (PAPP-A) & hormone (free β-HCG). Any abnormal levels may suggest a higher risk of a chromosomal abnormality in the fetus.
If a woman is identified as being at high risk for carrying a baby with a chromosomal abnormality based on the 1st-trimester screening, diagnostic testing is usually recommended, such as chorionic villus sampling (CVS) in the first trimester or amniocentesis in the second trimester. Even if a woman is not identified as high risk during the 1st-trimester screening, a 2nd-trimester screening is still offered. This screening involves more blood tests and checks for chromosomal abnormalities and neural tube defects, which helps confirm the results of the 1st-trimester screening.
Types of abnormalities associated with increased NT include
- Cardiac Abnormalities (congenital heart diseases)
- Diaphragmatic Hernia
- Skeletal dysplasia
- Neuromuscular Disorder

No comment